
Clinical, laboratory, and radiologic findings are reported in addition to treatment outcomes. Brainstem involvement was severe in some of the cases and was fatal in one patient. Here, we report the largest series of Caucasian patients with MOG-IgG-positive brainstem encephalitis so far. While the association of MOG-IgG with ON and myelitis is now well established, less is known about extra-opticospinal manifestations in MOG-IgG-related autoimmunity. Based on the fact that aquaporin-4 (AQP4)-IgG is usually absent in MOG-IgG-positive patients, that the histopathology of inflammatory CNS lesions differs between MOG-IgG- and AQP4-IgG-positive patients, and that MOG-IgG are pathogenic both in vitro and in vivo, MOG-IgG-related autoimmunity is now considered by many a disease entity in its own right, distinct both from classical MS and from AQP4-IgG-mediated neuromyelitis optica spectrum disorders (NMOSD). 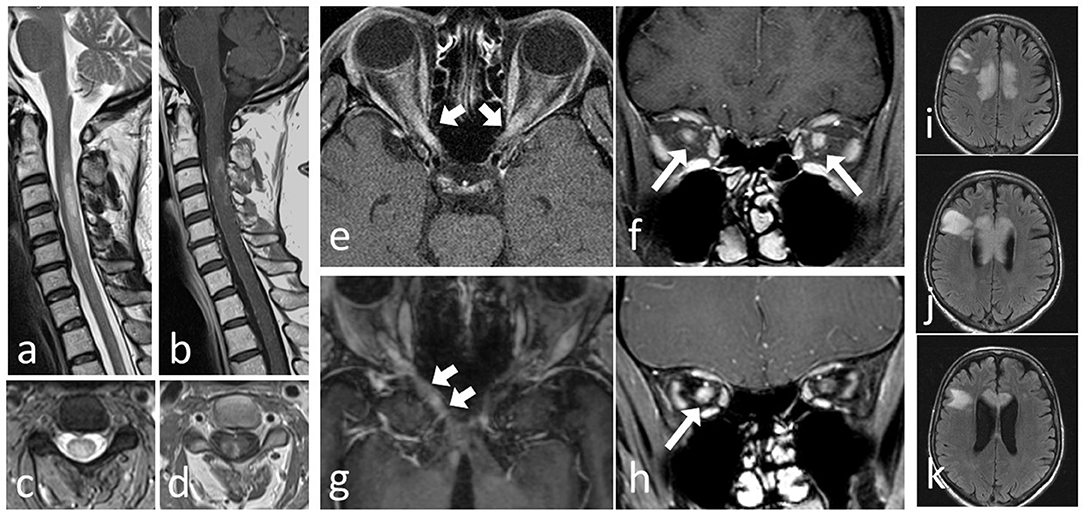
While MOG-IgG had initially been thought to play a role in classical multiple sclerosis (MS), recent studies have demonstrated that MOG-IgG are in fact a marker of autoimmune optic neuritis (ON) and (often longitudinally extensive) transverse myelitis. Over the past few years, a new diagnostic role has been found for antibodies to myelin oligodendrocyte glycoprotein (MOG-IgG) in adults. 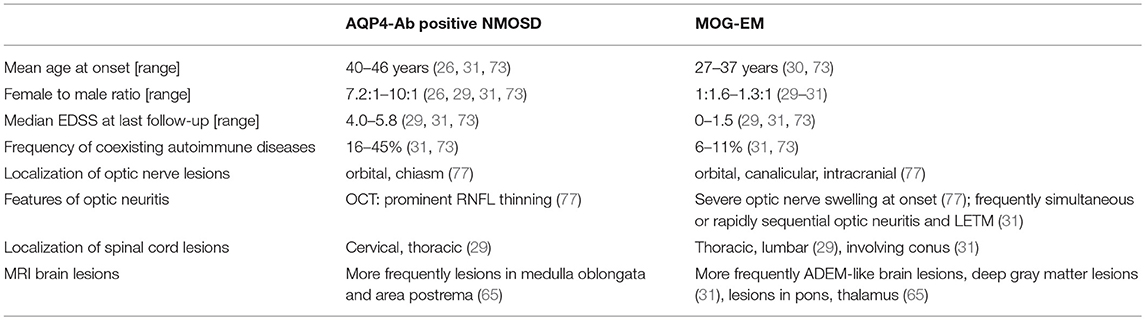 
As MOG-IgG-positive brainstem encephalitis may take a serious or even fatal course, particular attention should be paid to signs or symptoms of additional brainstem involvement in patients presenting with MOG-IgG-positive ON and/or myelitis. Clinical manifestations are diverse and may include symptoms typically seen in AQP4-IgG-positive neuromyelitis optica, such as INV and respiratory insufficiency, or in multiple sclerosis, such as INO. Conclusionsīrainstem involvement is present in around one third of MOG-IgG-positive patients with ON and/or myelitis. Brainstem involvement was associated with a more aggressive general disease course (higher relapse rate, more myelitis attacks, more frequently supratentorial brain lesions, worse EDSS at last follow-up). While one patient died from central hypoventilation, partial or complete recovery was achieved in the remainder following treatment with high-dose steroids and/or plasma exchange. Interferon-beta was followed by new attacks in two patients. Immunosuppression was not always effective in preventing relapses. The disease followed a relapsing course in 13/15 (87 %) the brainstem was involved more than once in 6. A history of teratoma was noted in one case. Attacks were preceded by acute infection or vaccination in 5/15 (33.3 %). Cerebrospinal fluid pleocytosis was found in 11/14 cases, with neutrophils in 7/11 (3-34 % of all CSF white blood cells), and oligoclonal bands in 4/14. MRI or laboratory signs of blood-brain barrier damage were present in 5/12. Lesions were located in the pons (11/13), medulla oblongata (8/14), mesencephalon (cerebral peduncles 2/14), and cerebellar peduncles (5/14), were adjacent to the fourth ventricle in 2/12, and periaqueductal in 1/12 some had concomitant diencephalic (2/13) or cerebellar lesions (1/14). 16/21 (76.2 %) brainstem attacks were accompanied by acute myelitis and/or ON. Brainstem inflammation was already present at or very shortly after disease onset in 7/15 (47 %) patients. Symptoms included respiratory insufficiency, intractable nausea and vomiting (INV), dysarthria, dysphagia, impaired cough reflex, oculomotor nerve palsy and diplopia, nystagmus, internuclear ophthalmoplegia (INO), facial nerve paresis, trigeminal hypesthesia/dysesthesia, vertigo, hearing loss, balance difficulties, and gait and limb ataxia brainstem involvement was asymptomatic in three cases. MethodsĪmong 50 patients with MOG-IgG-positive ON and/or myelitis, 15 (30 %) with a history of brainstem encephalitis were identified. To investigate the frequency, clinical and paraclinical features, course, outcome, and prognostic implications of brainstem involvement in MOG-IgG-positive ON and/or myelitis. Little is known so far about brainstem involvement in MOG-IgG-positive patients. Myelin oligodendrocyte glycoprotein antibodies (MOG-IgG) are present in a subset of aquaporin-4 (AQP4)-IgG-negative patients with optic neuritis (ON) and/or myelitis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
